From a trip to the grocery store to a visit to the dentist’s office, the most salient and lasting effects of the COVID-19 pandemic have impacted every aspect of our day-to-day activities. Once-familiar routines and interactions may seem more akin to maze-like challenges, requiring an unprecedented (and often daunting) degree of safety considerations and precautions to navigate. Given our still-developing understanding of the coronavirus and a nebulous timeline for a vaccine, it is clear these changes are here to stay. What we are experiencing is “the new normal.” For practices and patients to thrive, we must learn to accept and adapt.
The danger zone
While there is still much to learn about SARS-CoV-2, the virus that causes COVID-19, experts have agreed that the dental setting is a “uniquely risky environment.” Mark Wolff, dean of the University of Pennsylvania School of Dental Medicine, described dental practices as a “danger zone.” SARS-CoV-2 presents in the nasopharyngeal and salivary secretions of infected individuals and can be transmitted by breathing, talking, and coughing, among other methods. Dental care providers are at risk not only because they work in close proximity to the patient’s mouth, nose, and throat, but also due to their frequent use of aerosol-generating tools. Aerosols can cause virus particles to become airborne for up to several hours. When these particles eventually land on operatory surfaces, they remain an infection risk for an indefinite amount of time.
Due to the dangers these circumstances pose to providers and patients, and the initial uncertainty surrounding the mechanisms of viral transmission, nearly 200,000 dental practitioners in the United States ceased non-emergency care in the wake of the outbreak. Soon thereafter, the American Dental Association (ADA) and the Centers for Disease Control and Prevention (CDC) collaborated to establish guidelines for the safe reopening of dental practices across the country. By May 18, 2020, most practices were able to resume routine appointments and, as indicated by an ADA survey of 3,491 practices, 99.2% were open by late September (though 52.4% reported lower patient volume than usual).
The new routine
So, what does a routine preventive dental appointment look like under the new normal of COVID-19? The first change is apparent before a patient sets foot in the office. Approximately 24 hours before the appointment, the ADA recommends that patients be given a pre-screening call to assess their health status. This may include a questionnaire to determine if they have experienced any recent COVID-19 symptoms such as a fever or cough, as well as whether they may have been exposed through close contact with an infected person or travel to a high-risk area. During the call, patients may also be asked to limit the number of people who accompany them to the appointment and reminded to wear a mask.
After a patient arrives at the office, they have likely encountered a very different experience than those in previous years. Patients have been asked to wait outside until the staff is ready to see them, then have their temperature taken when they enter. Ideally, the waiting room is always close to empty. ADA president Dr. Chad Gehani reports that while his waiting room once had 14 chairs, now there are only four (one in each corner) and all toys and magazines have been removed. Additionally, the clipboard that patients use to fill out forms is sanitized between uses, writing implements are either wiped down or given to the patient to take home, and computer keyboards are covered.
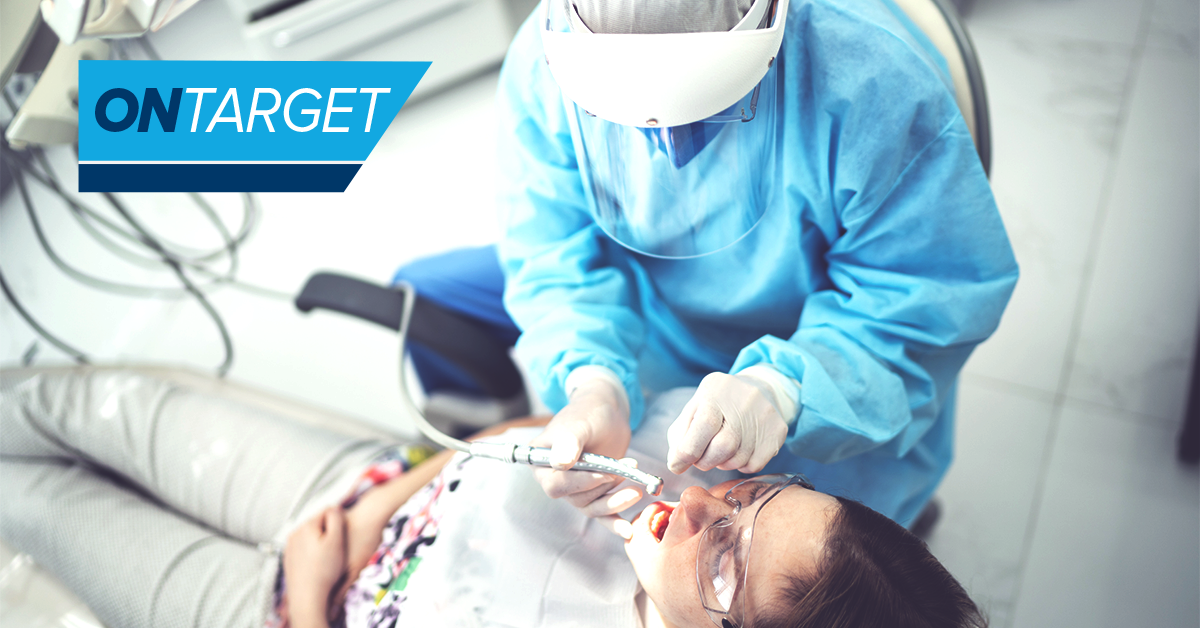
Personal protective equipment (PPE) has long been part and parcel of safe dental practice, but because of COVID-19, it has become more critical than ever. The ADA and CDC recommend that all patients and staff wear facemasks in the office and suggest that dentists don more PPE than usual when performing procedures. Pairing a face shield and goggles with PPE staples such as masks, gloves, and gowns can help reduce the chances of transmission.
In the operatory, tweaks to common preventive procedures also can halt the spread of COVID-19. While ultrasonic instruments are exceptionally effective at cleaning tooth surfaces, they also can aerosolize a virus. In their stead, many dentists are resorting to manual cleaning methods or, in some cases, products specifically designed to reduce airborne particles. Likewise, as saliva provides a vehicle for disease transmission, the combination of rubber dental dams and constant high-speed suction can minimize splatter and spray.
Post-appointment operatory cleaning and disinfection is standard infection prevention protocol for dental practices, but to mitigate the spread of COVID-19, some offices are taking the extra precaution of disposing and replacing all protective barriers after treating each patient. Other steps providers can take to protect themselves and their patients include rotating operatories between procedures, increasing office ventilation, and administering an antimicrobial pre-procedural rinse – a mixture of diluted hydrogen peroxide or iodine – to combat bacteria living in the mouth and upper throat. Though more research is needed to determine the efficacy of these steps, the consensus is that practices should enact every measure they can to prevent the transmission of COVID-19.
Teledentistry: Benefits and uses
The COVID-19 pandemic has seen many practices turn to teledentistry as a safe way to treat patients. Using a smartphone or computer and cloud-based platform, patients and providers can connect remotely and participate in face-to-face video calls, or virtual visits, as well as exchange vital information in the form of images, videos, and more.
Uses of teledentistry include:
- Problem-focused and urgent care evaluations (e.g., acute swelling/pain)
- Follow-up care after emergency visits
- Virtual triage for COVID-19 symptoms
- Referral to appropriate providers
Teledentistry can benefit dental practices and their patients by:
- Reducing nonessential visits
- Facilitating social distancing
- Mitigating potential infectious exposures
- Avoiding delayed preventive, chronic, or routine care
- Decreasing strain on office resources (by reducing PPE use, cleaning time, etc.)
- Assisting medically or socially vulnerable patients
- Preserving the patient-provider relationship
Looking ahead
The difficulties imposed on dental practices by COVID-19 are undeniable and significant: additional safety precautions before and after treatment can reportedly add up to 30 minutes to each appointment and limit the number of patients dentists can treat daily. Couple this with other pandemic-related factors that lead to a decrease in patient visits (such as personal, health, or economic concerns), and it becomes inevitable that many dentists are concerned about the sustainability of their practices.
Dentistry is a profession centered around health and grounded in long-standing infection prevention protocols, so it seems more than well-equipped to survive and thrive in this new reality.
Selected references
Health Policy Institute and American Dental Association. COVID-19: Economic impact on dental practices week of September 21 results.
Patient Safety Network. COVID-19 and dentistry: Challenges and opportunities for providing safe care. August 31, 2020.
Wei-Haas M. How to safely go to the dentist during the pandemic. National Geographic. September 8, 2020.
Centers for Disease Control and Prevention. Using telehealth to expand access to essential health services during the COVID-19 pandemic. June 10, 2020.
– – –
This blog post originally appeared in OnTarget. To read the latest issue and view current promotions, visit pattersondental.com/dental/ontarget.



One thought on “Dentistry and COVID-19: The New Normal Is Here”
Comments are closed.