The dental waterlines have been tested; what are the next steps and what do you do with the test results? In part three of our water series blog we examine when and how to remediate failed waterlines, differentiate between shock and waterline maintenance treatments, and discuss recommendations for retesting. Proper implementation of a waterline maintenance protocol is a critical component of any comprehensive water management program. This step is key to the success in maintaining safe bacterial levels in dental unit waterlines.
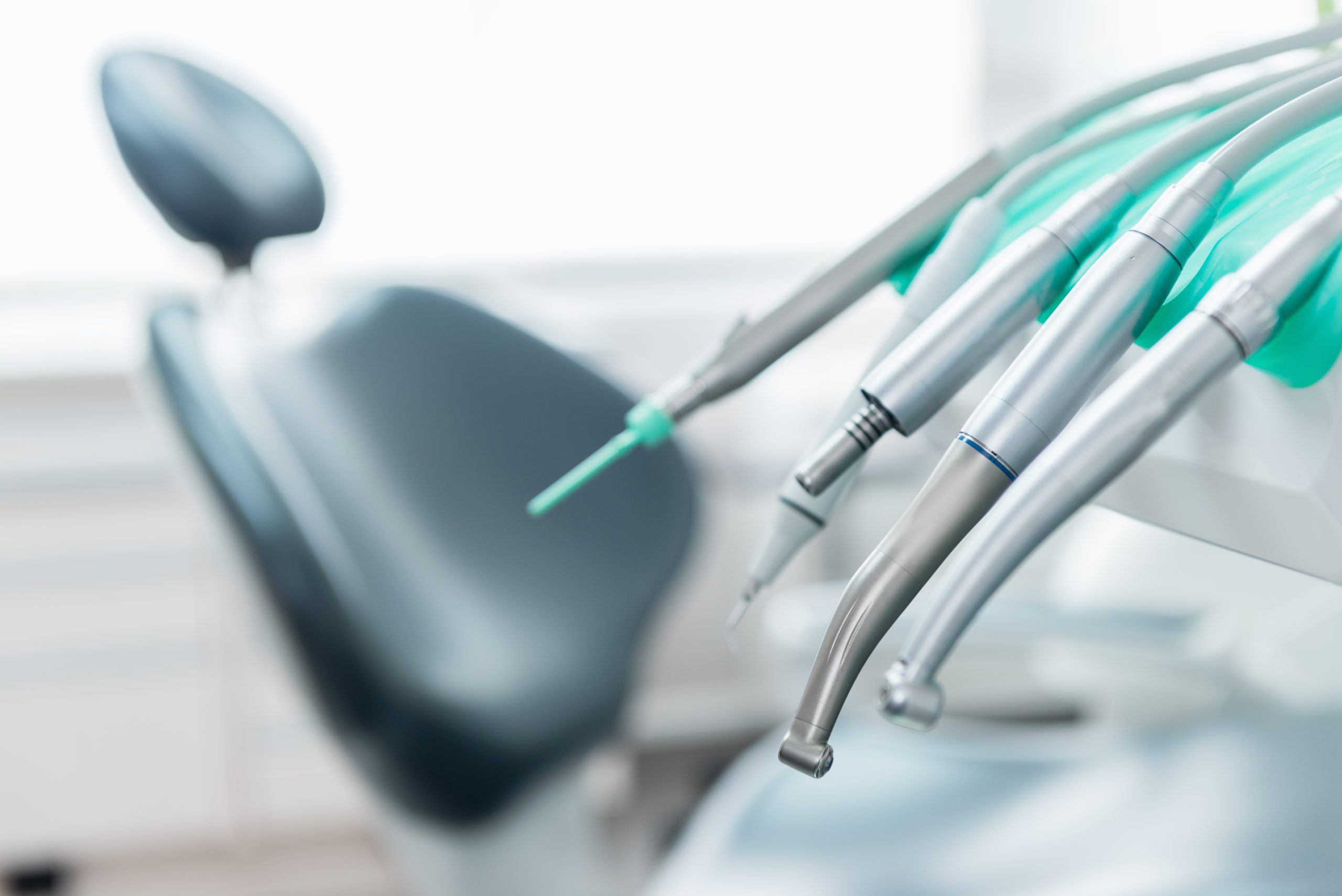
Dental Unit Waterline Chairside Testing
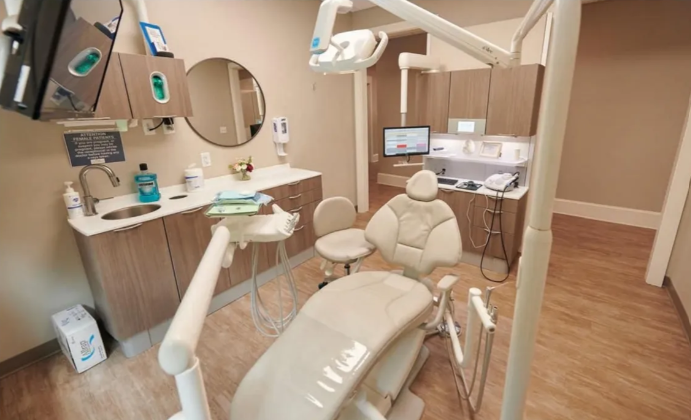
Dental Infection Control Awareness Month: Spotlight on Waterline Safety
This article first appeared in OnTarget, but we thought it would be great to share this important information once again.
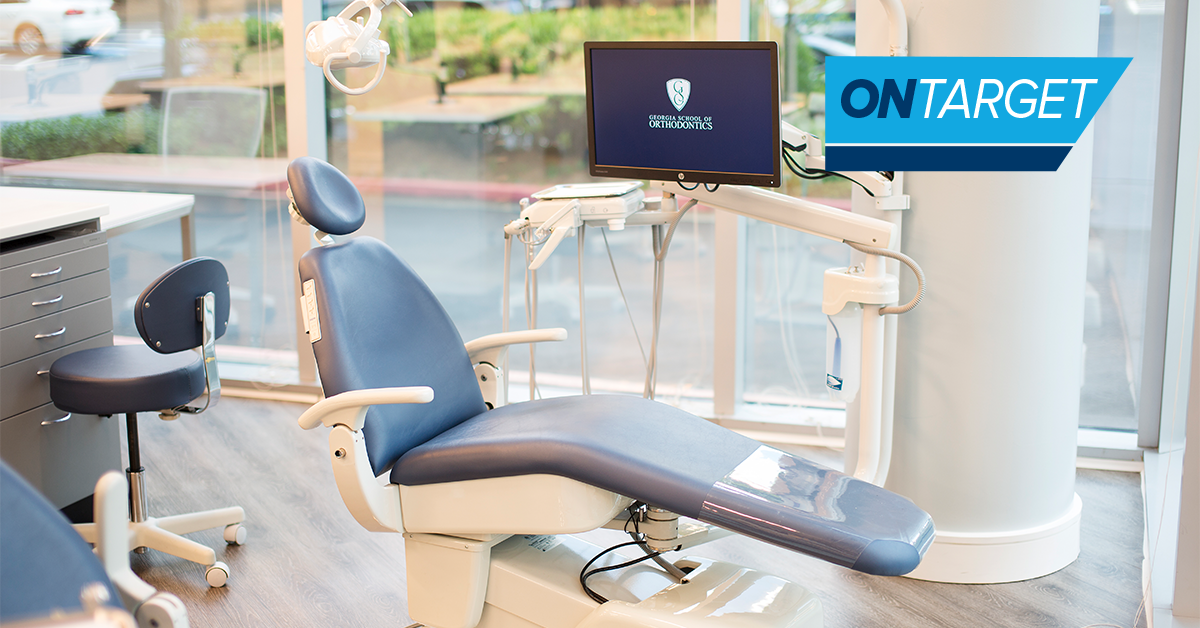
OnTarget Highlight: Preventing and Treating Peri-Implantitis
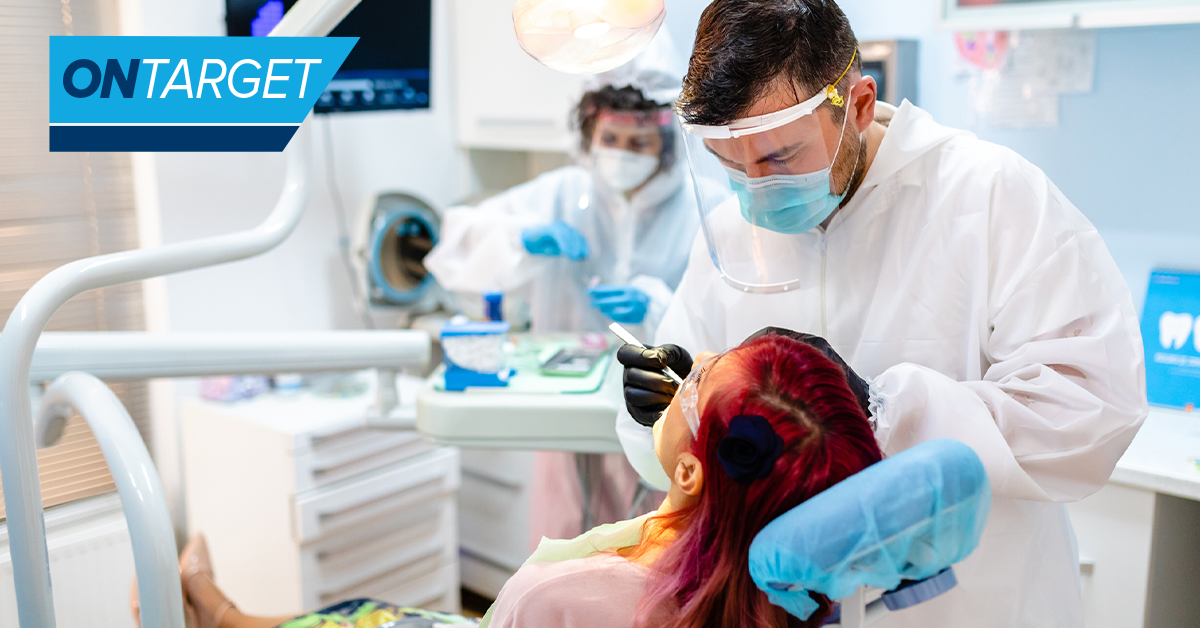
Brush up on hand hygiene for Global Handwashing Day
Proper hand hygiene is the most important step dental practices can take in the name of infection control and prevention. For Global Handwashing Day, we examine the history, challenges and best practices for hand hygiene in the dental setting.
A look back at COVID-19: Lessons learned from the height of the pandemic
Although COVID-19 still poses threats, much of what dental practices put in place during the early days of the pandemic continue to demonstrate important lessons about infection control and prevention, issues that have become paramount and will continue to be critical moving forward.
The importance of safe dental instrument processing
Proper instrument processing not only extends the lifespan of your valuable investments but also helps ensure the safety of your patients and staff.
Creating a culture of safety at your dental practice
A team commitment to infection prevention ensures the health, safety and satisfaction of your patients and staff while protecting your practice from costly repercussions.
Combating cross-contamination in the dental setting
Maintaining a safe, infection-free practice means avoiding cross-contamination whenever possible. Here are some best practices for proper hand hygiene, instrument processing and surface asepsis prevention.
Linda Harvey: 3 Common Misperceptions on OSHA’s Emergency Temporary Standard (ETS)
Compliance consultant Linda Harvey shares three common misperceptions regarding OSHA’s recently issued ETS for protecting health care workers from the coronavirus.
Dental Unit Waterline and Evacuation System Safety
Dental unit waterlines (DUWLs) and evacuation systems are an invaluable asset in the dental operatory. But evacuation lines can become a source of cross-contamination because they serve as ideal breeding grounds for biofilm. To ensure safe DUWL use, dental professionals must adopt a three-pronged approach to battle biofilm at its source.
Linda Harvey: The Air That You Breathe in Your Practice [VIDEO]
Air quality has been a hot topic for a long time and COVID-19 has further illuminated the focus on aerosols in the dental setting. This video from Linda Harvey, RDH, dives into what you can do to be safe and achieve higher quality air in your practice.
10 Steps to Promote a Culture of Patient Safety
While patient safety has long been paramount to modern dentistry, the newest challenges posed by COVID-19 have inspired many practices to review their policies and procedures. To help promote patient safety, the American Academy of Pediatric Dentistry (AAPD) has created a list of recommendations.
Dentistry and COVID-19: The New Normal Is Here
Given our still-developing understanding of the coronavirus, it is clear changes to our daily life are here to stay. What we are experiencing is “the new normal.” For practices and patients to thrive, we must learn to accept and adapt.
Oral Health Professionals: Meeting the Risks of COVID-19
After the initial outbreak of COVID-19 shut down almost 200,000 dental practices in the United States in early 2020, the industry needed to quickly develop an effective response that would not only allow practices to reopen safely but also ensure that patients could access the oral care they needed.
Proper Hand Hygiene in the Age of COVID-19
Hand washing, though it may seem simplistic during a pandemic, can actually be the most effective way of preventing the spread of germs, including those that cause COVID-19. As dental practices navigate the recent challenges related to COVID-19 and work to implement strategies to protect patients and staff, a closer look at hand hygiene may prove helpful.
8 Ways to Improve Your Dental Practice’s Organization
Integrating these tools and strategies will improve practice efficiency and impress upon your patients how important their comfort and safety are to you.
Building and Supporting a Robust Culture of Safety in the Dental Workplace
Infection control and adherence to strict regulations are critical components in the success of a dental practice. It is up to dental office leaders to create and sustain a culture of safety involving the entire dental team.
Dental Instrument Reprocessing and Waterline Maintenance: Behind the Scenes
Safety is a critical part of every dental patient’s experience. They want to feel comfortable about the care you and your team provide, and that includes the steps you take to ensure they’re safe from infection. What patients see in your waiting room and operatories is only part of the story. Would they still feel good about your practice if they looked into your sterilization room or could inspect your dental unit waterlines?
Equip Your Dental Practice with Next-Level Sanitization with PurLite Clean UV-C Cleaner
Keeping high-touch personal items and PPE clean can provide additional safeguards against the spread of COVID-19. One solution for sanitizing high-touch personal items is the new PurLite™ Clean UV-C Cleaner. PurLite is a sanitizer that uses advanced, medical grade UV-C technology to provide a fast and effective way to ensure patients and employees feel safe and protected while in your office.
The Three Ps for Infection Prevention [Audio + Resource Guide]
Undeniably, COVID-19 has forever changed the way we practice dentistry and manage infection control. Every area of your practice has been impacted, from how patients are scheduled and checked in, to how office staff don and doff all the new PPE.
A Quality Assurance Approach of Infection Prevention from OSAP [Part 2]
In part two of its series “Implementing Routine Quality Assurance of Infection Prevention Policies and Procedures,” OSAP continues its close look at instrument reprocessing. Specifically, part two in this series outlines one approach to performing routine quality assurance related to packaging instruments during reprocessing.
Failure to replace: Who pays the ultimate price?
The current recommendation for when to replace a scaler is when 20% of the instrument blade width or length is reduced or no longer the original design. But how long it takes for each instrument to reach this threshold is dependent on several factors. Deb (Hume) Brown, RDH, shares some of these factors and how a failure to replace instruments can affect the clinician and the patient.
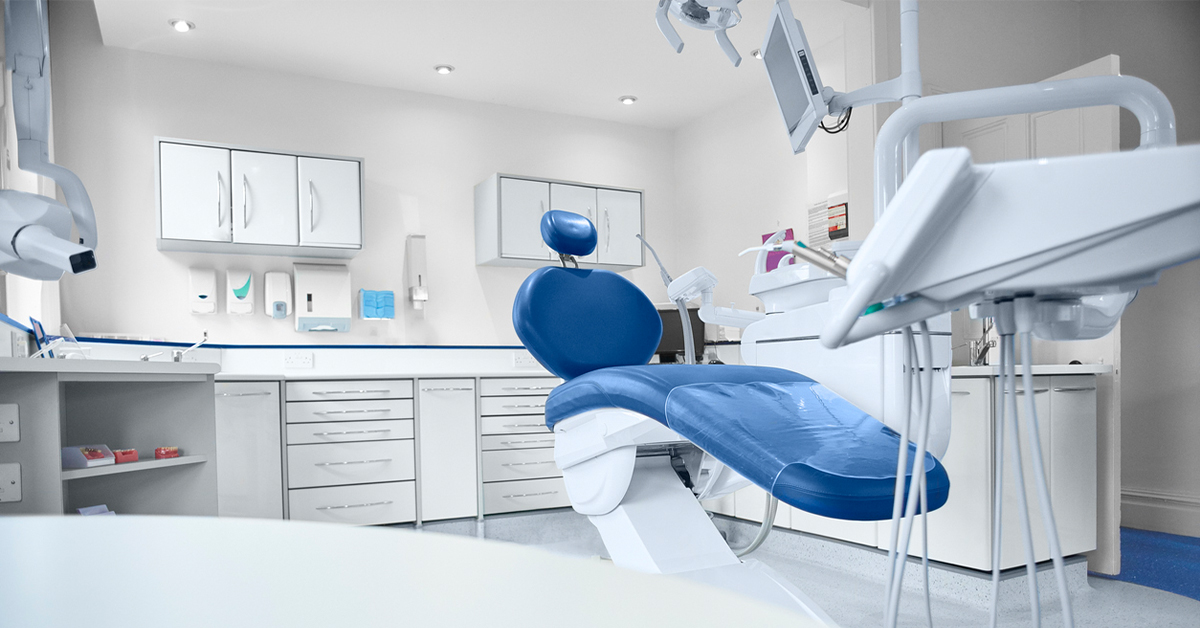
Boost Patient Confidence with Sterilization Solutions from A-dec
As dental practices continue to examine infection control guidelines to meet the demands of the ongoing coronavirus pandemic, it’s important to consider how patients will feel as they walk into your office. A-dec has many solutions to not only improve the safety of your office, but also to visually show patients you’re keeping their health at the forefront.
A Quality Assurance Approach of Infection Prevention from OSAP
As dental practices continue to evaluate office policies and procedures during the ongoing coronavirus pandemic, infection control will continue to be an important area of focus. To that end, the current issue of Infection Control in Practice by OSAP dives into creating an effective infection prevention and control program for your practice.
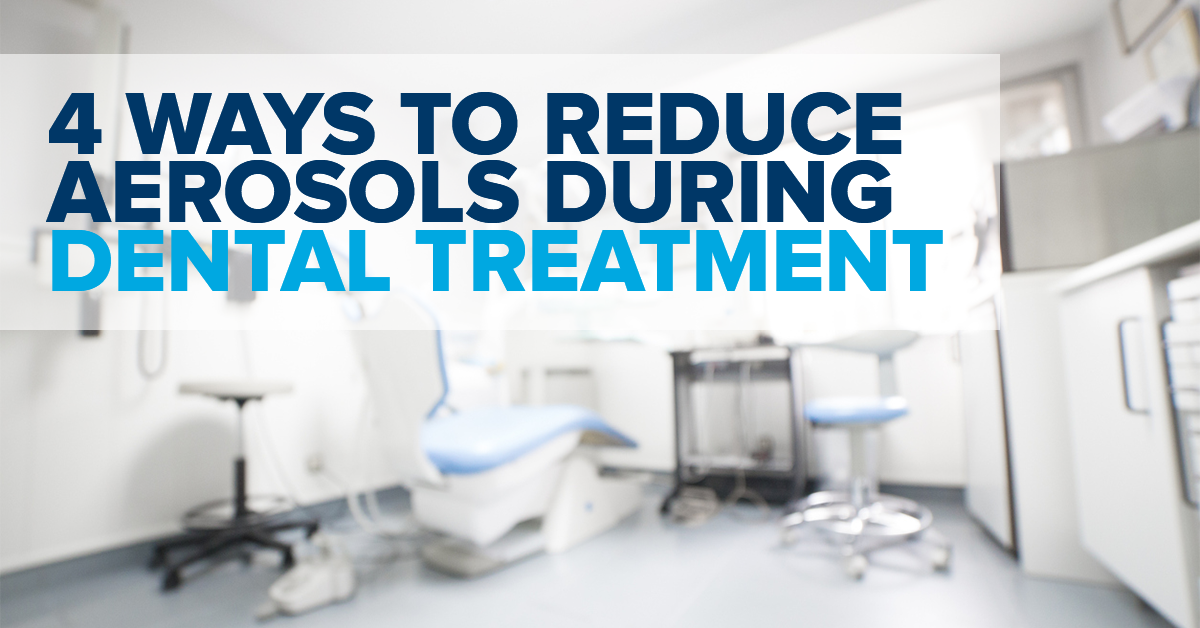
4 Ways to Reduce Aerosols During Dental Treatment
As we reenter the practice world, one question dominates every conversation. How do we best reduce the aerosol generated during dental treatment? David Rice, DDS, shares four ways you can keep you, your team and your patients safe.
Keeping Staff and Patients Safe: Personal Protective Equipment and Donning and Doffing Advice
Nothing is more important than protecting the lives of your patients and staff. Yet new circumstances you and other dental professionals are now facing require the use of more personal protective equipment (PPE) and the proper procedures for ensuring you and your team are securely covered – from head to toe.
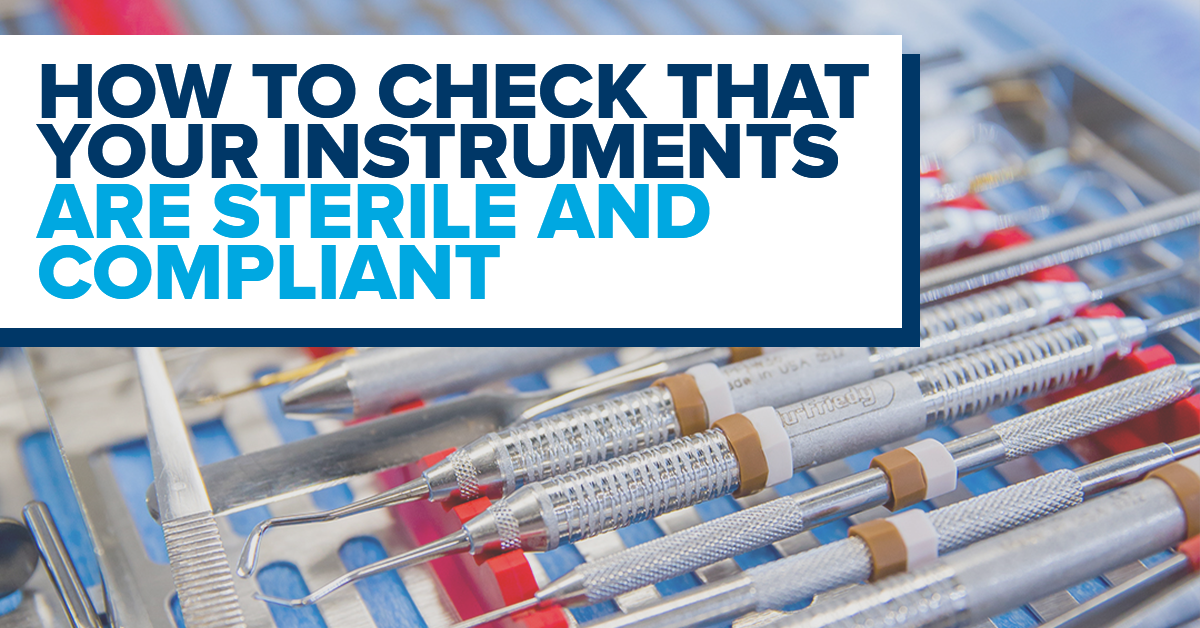
How to Know Your Instruments Are Sterile and Compliant
Cleaning and sterilizing dental instruments for re-use can be tedious and dull, but the task is a crucial component to ensuring the safety of staff and patients. Further, ensuring that instruments are free of potentially infectious material and debris is critical to the quality care that dental health professionals pledge to provide. Gain a better understanding of this importance and see how to set up an easy-to-maintain compliance program in this guest post from Hu-Friedy.
On-Demand Webinar: Respiratory Precautions and Aerosol Management Solutions
Managing respiratory risk is critical as dental practices begin resuming regular care amid COVID-19. In this on-demand webinar, OSAP and Patterson Dental discuss current respiratory precautions and aerosol management solutions from an equipment and technology standpoint for dental practices.
Critical Compliance Factors as You Reopen Your Dental Practice
A growing number of states are allowing businesses, including dental practices, to reopen. Is your practice ready to resume routine patient care? Linda Harvey, RDH, shares several compliance factors to consider as part of your reopening process.











![Linda Harvey: The Air That You Breathe in Your Practice [VIDEO]](https://www.offthecusp.com/wp-content/uploads/2021/05/MicrosoftTeams-image-4.png)






![The Three Ps for Infection Prevention [Audio + Resource Guide]](https://www.offthecusp.com/wp-content/uploads/2020/09/infection-control-1200x628-iStock-1253398698.jpg)
![A Quality Assurance Approach of Infection Prevention from OSAP [Part 2]](https://www.offthecusp.com/wp-content/uploads/2020/08/osap-infection-control-autoclave-dental-sterilization-1200x628-iStock-1025299028.jpg)