Review how to maintain regulatory compliance and a high standard of care when providing this valuable service.
Patient-Led Financing: Getting Patients to “YES”
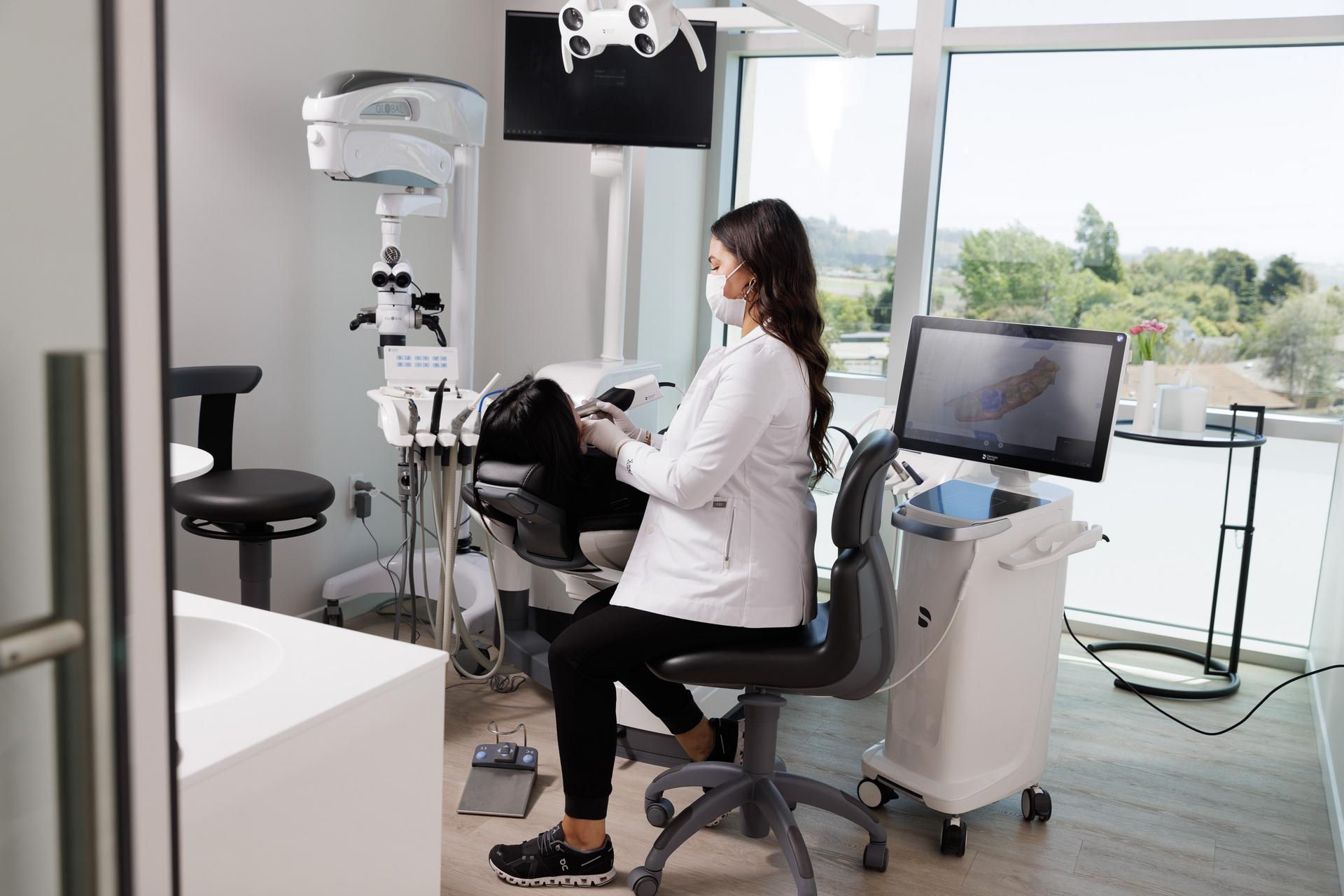
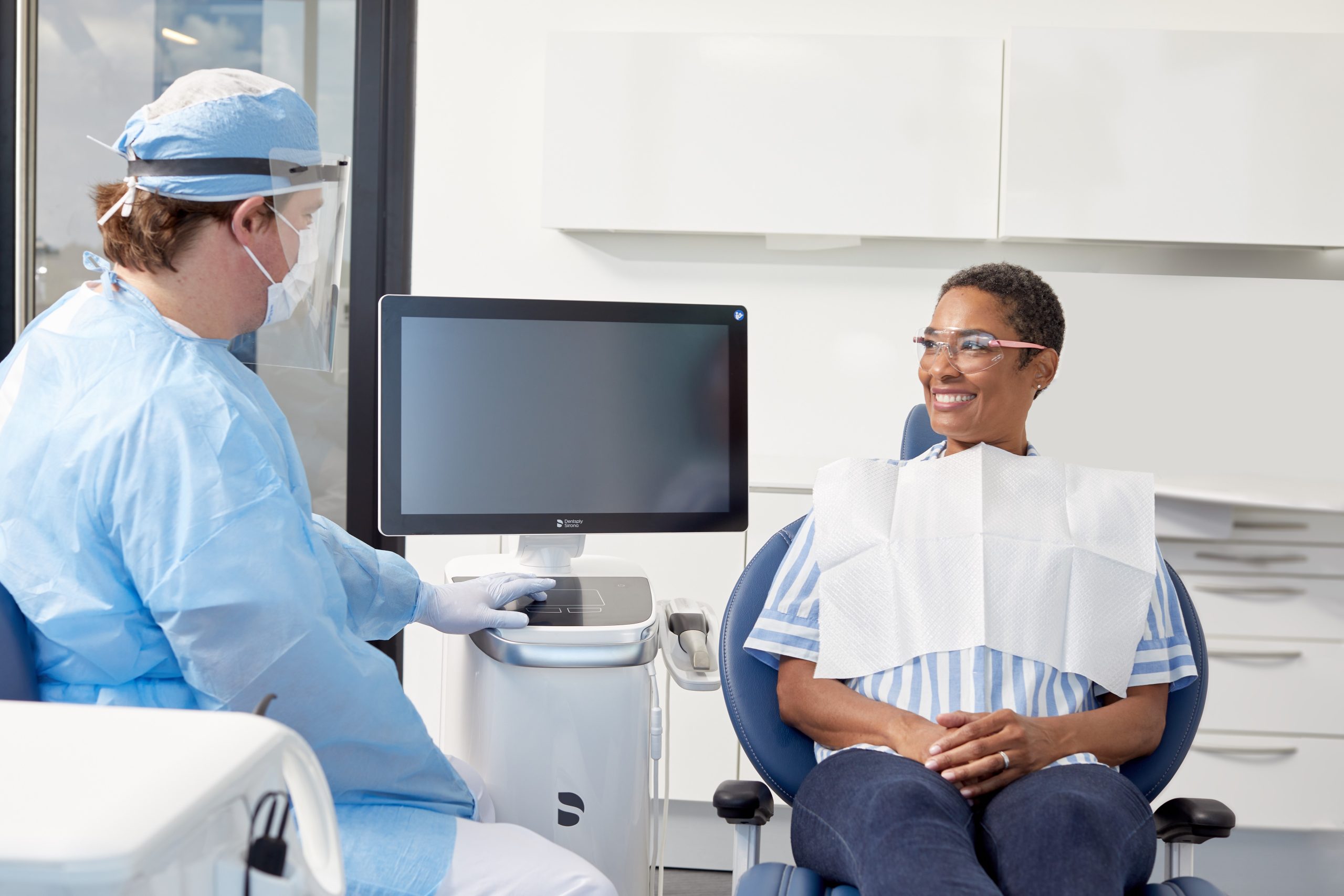
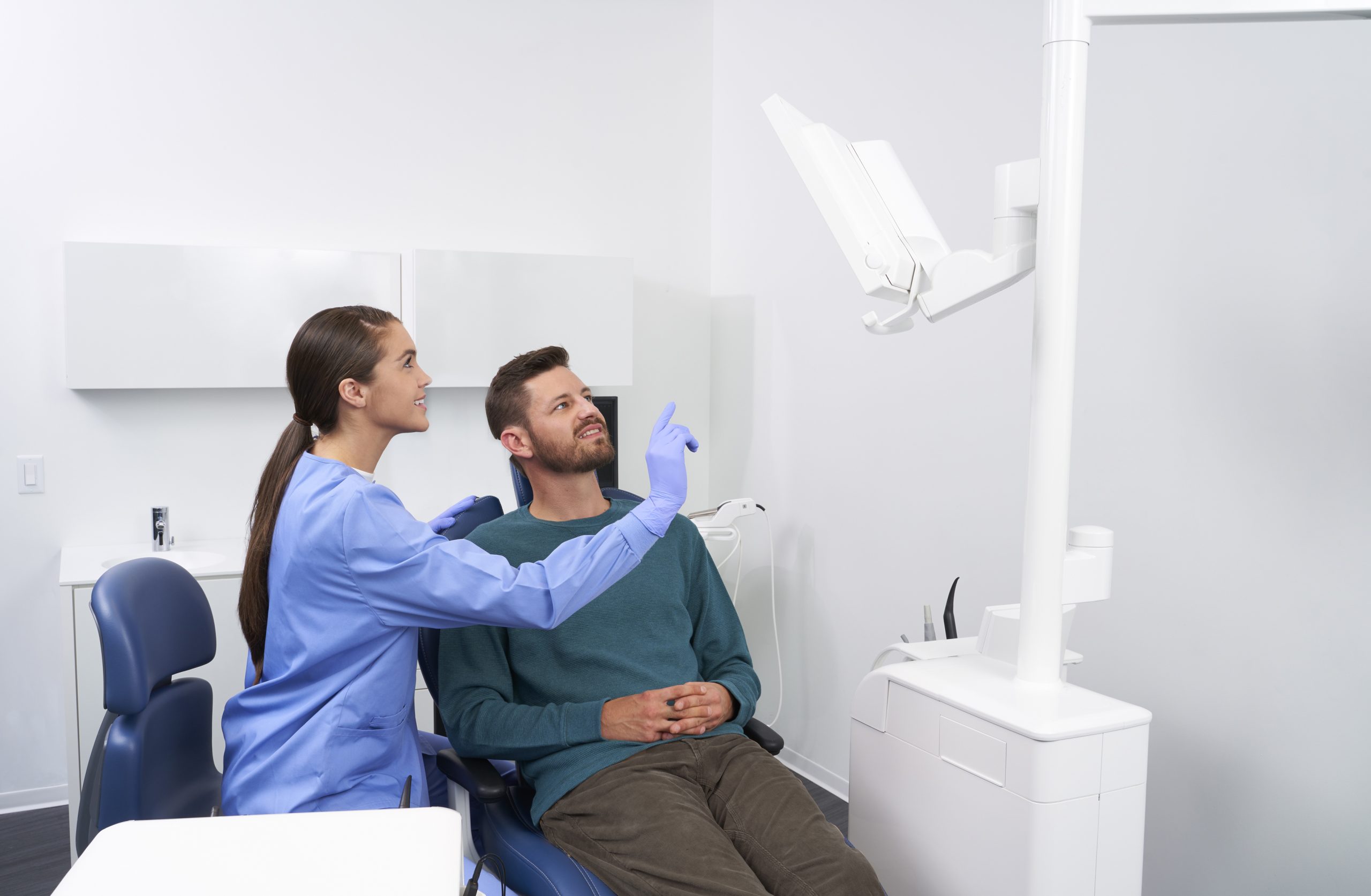
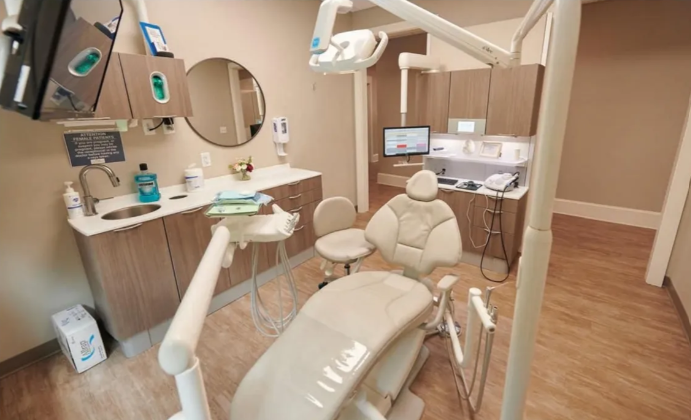
Building a Practice Around a Vision of Superior Patient Care
Kincaid Dental Center invested in technology and comfort to improve the patient experience and is seeing rapid growth as a result.
“The Cloud”: A Primer
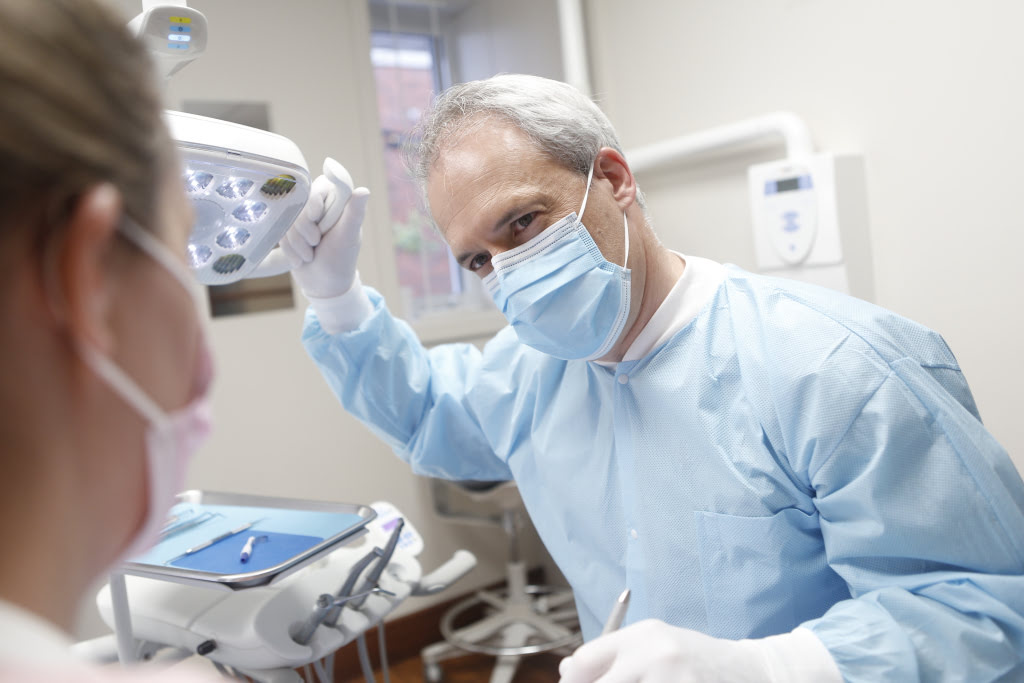
Developments in Dentistry
2024 saw dentists continue to bring new, high-value services to their practices. Read on to review some of the key trends and innovations that are transforming modern dentistry.
Teledentistry: Challenges & Opportunities
Using technology to deliver dental care can offer both providers and patients an unprecedented level of convenience, but there are several challenges dentists must address to ensure success.
Patient Convenience: 6 Tips to Boost Loyalty to Your Practice
Don’t Lose Focus: Your Hygiene Team Needs Attention
Success in the Cloud: Benefits for Multilocation Practices
Celebrating National Brush Day: How Dental Teams Can Make an Impact
Bring Your Practice to the Next Level Without Getting Buried in Work
Office Managers: A Glowing Review
The Benefits of Next-Gen Midmark Sterilizers
See why next-generation Midmark sterilizers are a smart investment.
Dental Infection Control Awareness Month: Spotlight on Waterline Safety
This article first appeared in OnTarget, but we thought it would be great to share this important information once again.
Why Dentists Are Choosing Chloroprene Gloves: The Perfect Balance of Comfort and Protection
Join Us at Solea Summit 2024
Why Considering Price Alone May Come at a Cost
Choosing the right PPE is essential to making dental care safe and comfortable for both staff and patients. While budgetary constraints can make it tempting to select items such as medical gloves and masks based primarily on price, this approach can be far more costly in the long run.
Care Beyond the Chair: A Trusted Provider for All Patients
5 Ways to Show Your Office Manager They’re A Rockstar
In honor of Office Manager Appreciation Month, we’ve gathered a list of ways to honor these everyday heroes like the rockstars they are. Plus, we’re giving away a $500 Spafinder Gift Card to one lucky office manager!
4 Ways to Increase Case Acceptance & Practice Efficiencies
5 Common Business Mistakes in Dental Practices
Elevate Patient Engagement with a Scan
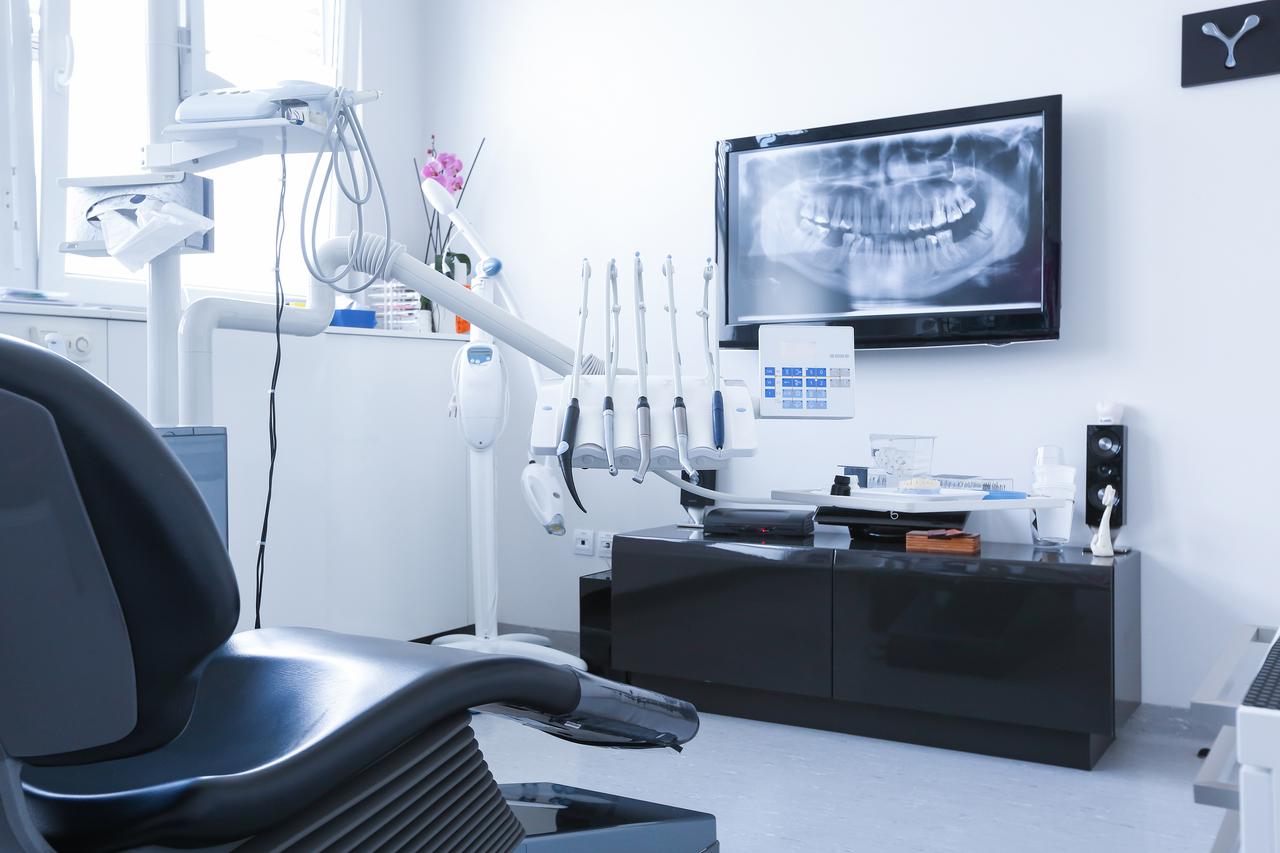
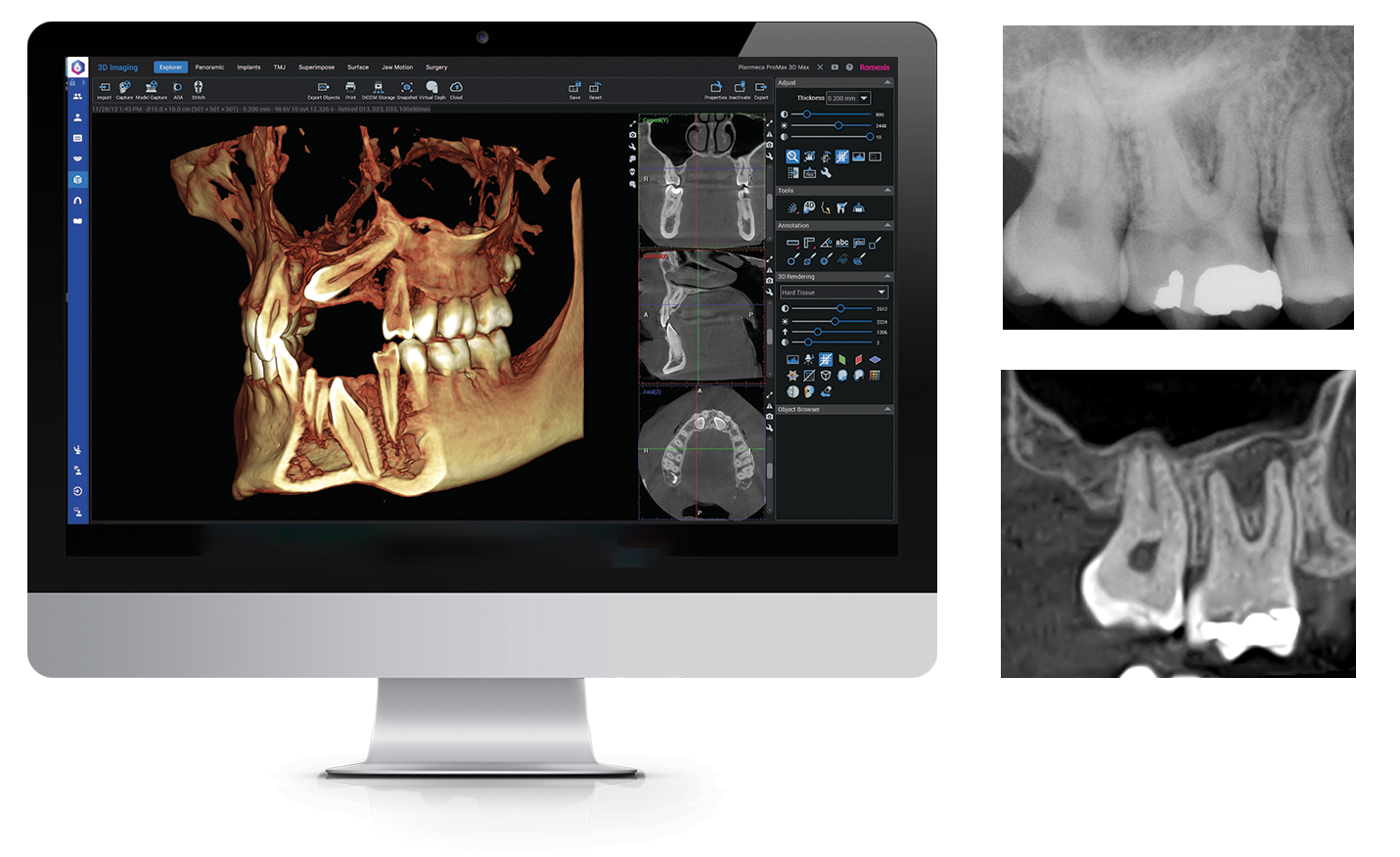
How to Choose Your Diagnostic Imaging Technology
Content provided by Planmeca
Upgrade to Eaglesoft Version 24.00 Today
Multilocation Eaglesoft Users – is it Time to Expand Your Software Horizons?
Set the Tone: How to be a Positive Leader for Your Dental Practice
TBS Dental Trade in Program – Trade Up, Give Back
Selling a Dental Practice for Maximum Value
Primeprint™ Solution – 3D Printing Simplified
Content provided by Dentsply Sirona.